If you’ve recently been told you have calcific tendinopathy, you’re likely in pain, confused by your scan results, and unsure of what to do next. Maybe your doctor mentioned “calcium in the tendon,” or you’ve been offered an injection or even surgery. Understandably, that can feel overwhelming.
The good news? This condition is usually treatable without surgery, and with the right support, most people make a full recovery.
Let’s walk you through what’s really going on — and how we can help.
💡 What Is Calcific Tendinopathy?
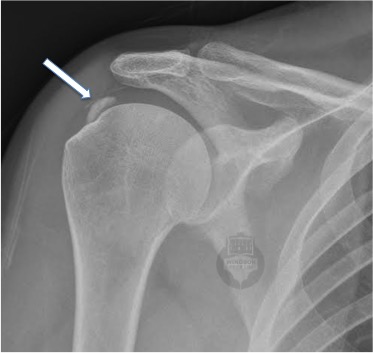
Calcific tendinopathy occurs when calcium deposits build up inside a tendon — most often in the shoulder (particularly the supraspinatus tendon). It’s not the same as a tendon tear, and it doesn’t mean your tendon is “turning to bone.”
It’s actually a biological process, not just the result of wear and tear. It typically progresses through a few key phases:
- Pre-calcific phase – tendon cells start behaving abnormally
- Calcific phase – calcium crystals form inside the tendon
- Resorptive phase – your body starts breaking the calcium down (this is usually when pain peaks)
- Post-calcific phase – healing and tissue remodelling
You might not feel anything for months — then suddenly, your shoulder becomes painful, stiff, and hard to sleep on.
🔥 Why It Hurts (Especially at Night)
Pain often spikes during the resorptive phase, when your body is actively trying to break down the calcium deposit. That process can trigger intense inflammation inside the tendon and surrounding tissue.
Common symptoms include:
- Sharp or aching pain in the front or top of the shoulder
- Difficulty lifting the arm, especially overhead
- Pain at night, especially lying on the affected side
- Reduced range of motion and strength
You’re not imagining it — and you’re not to blame. This isn’t the result of poor posture or lifting something the wrong way. It’s a condition that often develops silently over time.
🧬 What Causes It?
It’s Not Just Overuse
While repetitive stress may play a role, the main drivers are biological, not mechanical. Here’s what current science tells us:
- Tendon cells (tenocytes) may transform into cells that behave more like bone-forming or cartilage cells — this is called metaplasia
- Poor blood supply (common in certain areas of tendons) and local tissue stress may contribute
- It’s more common in women aged 30–50, suggesting a possible hormonal link
- There may also be a genetic predisposition in some people
📚 Uhthoff & Loehr, J Am Acad Orthop Surg, 1997
Inflammatory Conditions Like Crohn’s Can Play a Role Too
Emerging research has shown a connection between Crohn’s disease and calcific tendinopathy. That’s because chronic inflammation from autoimmune or gut-related conditions can affect tendons — not just joints.
If you have Crohn’s (or another inflammatory condition), your tendons may be more vulnerable to abnormal calcium buildup due to systemic inflammation.
📚 Chandrashekara et al., Rheumatol Int, 2020
🔍 What We See on Scans
- X-rays are excellent for showing the location, size, and stage of the deposit.
- Ultrasound is even more helpful because it allows us to see how dense or soft the deposit is — and it’s especially important if we’re considering a guided procedure.
- In some persistent cases, we may recommend an MRI or CT to rule out other issues.
Remember: the amount of calcium doesn’t always match the amount of pain. A small deposit can be very painful if it’s inflamed, and a large one might be completely silent.
🛠️ What Actually Works? (Evidence-Based Treatment)
Most people do not need surgery. Here’s the step-by-step approach we use — based on the latest research and years of clinical experience.
✅ Step 1: Settle the Pain, Support the Tendon
This is where we start for nearly everyone:
- A short course of anti-inflammatory medication (if safe for you)
- Relative rest from aggravating activity — not total immobility
- A targeted physiotherapy plan, including:
- Range of motion exercises
- Postural control and scapular strength
- Tendon-loading exercises to help tissue adapt
This phase aims to reduce inflammation and restore movement — usually enough to resolve symptoms in 2 out of 3 people within a few months.
✅ Step 2: Image-Guided Interventions (If Needed)
If pain persists beyond 6–12 weeks or if movement is severely limited, we might consider:
💉 Ultrasound-Guided Lavage (Needling)
Using real-time ultrasound, we insert a fine needle to break up and flush out the calcium deposit. It’s done under local anaesthetic, takes about 20 minutes, and can significantly reduce pain — especially during the soft/resorptive phase.
💥 Shockwave Therapy
This uses mechanical pressure waves to break up the deposit and stimulate healing. While it’s less targeted than needling, it can be helpful in chronic cases when combined with rehab.
⚠️ Step 3: Surgery (Only as a Last Resort)
Surgery is rarely needed, but it may be considered if:
- Symptoms persist for more than 6 months
- There’s significant pain or functional loss
- Non-surgical care hasn’t worked
Minimally invasive arthroscopic surgery can remove the deposit, and outcomes are generally good — but this is typically a last step, not the first.
🏋️♀️ The Role of Physiotherapy
Physiotherapy isn’t just a passive treatment — it’s your roadmap to long-term recovery.
We help by:
- Reducing pain through gentle movement and load management
- Restoring range of motion and tendon strength
- Improving shoulder mechanics and confidence
- Supporting recovery after a procedure or surgery (if needed)
Whether your goal is to get back to work, gym, or just sleep comfortably — we tailor the plan to you.
🧠 Final Thoughts
Calcific tendinopathy might sound serious, but in most cases, it’s completely treatable. The calcium deposit often shrinks or is reabsorbed naturally over time. The pain can be managed. And most importantly, you’re not stuck with this forever.
With the right guidance, a clear plan, and someone in your corner — you can get through this and come out stronger on the other side.
✅ Ready to Feel Better?
If you’ve been diagnosed with calcific tendinopathy and you’re unsure what to do next — we’re here to help.
At Melbourne Shoulder Rehab, we take the time to explain your condition, tailor your treatment, and guide you through a recovery plan backed by the latest research.
Whether you’re in the early stages of pain or considering more advanced treatment options like ultrasound-guided needling, our team can support you every step of the way.
👉 Book an appointment today to get clarity, relief, and a pathway forward.
